Is Chronic Kidney Disease Becoming a Silent Killer Globally?
Published on 27 Jan, 2022

Chronic kidney disease (CKD) and associated risks can cause irreversible damages that could prove fatal for the patient. The rising incidences of CKD is not only affecting global health but also leading to adverse societal and economic consequences. However, timely and effective strategies can help in correct management of the disease and control its spread.
Introduction
According to Dr. Theo Vos, Professor of Health Metrics Sciences at the Institute for Health Metrics and Evaluation at the University of Washington School of Medicine, “Chronic kidney disease (CKD) is a global killer hidden in plain sight.” Approximately 700 million people around the world have been affected by CKD. “The evidence is clear,” he confirmed. “Many nations’ health systems cannot keep pace with the dialysis demand. Cases far exceed and are well beyond the ability of those systems to handle. The consequences, literally, are deadly.”
The statement is based on a scientific study on global, regional, and national burden of CKD, which showed that the need for dialysis has increased ~40% since 1990. Unfortunately, access to this life-saving treatment is challenging for the common people.
CKD at a glance
The kidney, an essential organ in the human body, filters excess fluid and waste products from the blood. If the kidney is unable to function normally, it is termed as CKD or chronic kidney failure. A few nonspecific signs and symptoms (e.g., nausea, vomiting, loss of appetite, fatigue and weakness, muscle cramps) crop up in the early stages of CKD. As the progression of kidney damage is slow, the actual symptoms develop over a long time period. When the kidney loses its ability to function properly, fluid begins to accumulate in the lungs, causing shortness of breath and chest pain. CKD is categorized into five stages based on the functioning of the kidney, where stage 1 indicates normal kidney function and stage 5 indicates kidney failure.
Associated risks
CKD is a silent disease that makes its detection difficult in the early stages as most of its symptoms are common. Due to late detection, issues associated with kidney failure reach towards the advance stage and progresses with irreversible damage. Lack of proper kidney function leads to the problems of fluid build-up, excess body waste, and electrolyte imbalance. Complications due to CKD includes gout (also known as hyperuricemia, which is caused by excess uric acid in the body), anemia (lack of red blood cells), metabolic acidosis (imbalanced quantity of acids), bone disease, hyperphosphatemia (elevated level of phosphate in the blood), hyperkalemia (high potassium level), and other similar health issues. As the body is unable to eliminate the excess fluid, chances of fluid overload increase, which can cause severe heart- and lung-related issues and even lead to congestive heart failure.
Impact of CKD on global health
A Global Burden of Disease study (published in 2017) includes the global, regional, and national estimation of morbidity and mortality related to CKD and impaired kidney function. CKD has 9.1% (697.5 million cases) of global prevalence, in which India and China top the list with 115.1 million and 132.3 million cases, respectively (nearly one-third of total). Moreover, there is a surge in the number of all-age global incidence of dialysis and kidney transplantation. In addition, the rate of dialysis and transplantation increased 43.1% and 34.4%, respectively, between 1990 and 2017, which also reveals the availability and accessibility of the therapies. CKD was responsible for causing 1.2 million deaths worldwide in 2017 (12th leading cause), with another 1.4 million deaths attributed to cardiovascular disease (CVD) developed due to impaired kidney function. While the mortality rate of other chronic diseases (CVD, COPD) decreased from 1990 to 2017, the global all-age CKD mortality rate went up 41.5%, which is a matter of grave concern.
Societal and economic impact of CKD
The findings of the study emphasize the association between increased healthcare cost and reduced life quality with the progression and advancement of CKD stages. A linear increment emerges between the utilization of healthcare facilities and individual-level economic burden over the period of early to advanced stage CKD. Progressing to the point of no return of end-stage CKD, the increment of cost becomes high, based on the requirement of frequent dialysis and associated therapies. However, the early and moderate stages are becoming the most costly and important ones at the societal level, as the number of CKD patients is rising. Disease progression and patient survival mainly depend on effective management. This is a societal menace as, with growing elderly population, more patients would progress to advance, resource-intensive stages of CKD. Moreover, in low- and middle-income countries, lack of access to dialysis would increase premature mortality (younger people suffering from CKD), which would result in a diminished labor force and poverty.
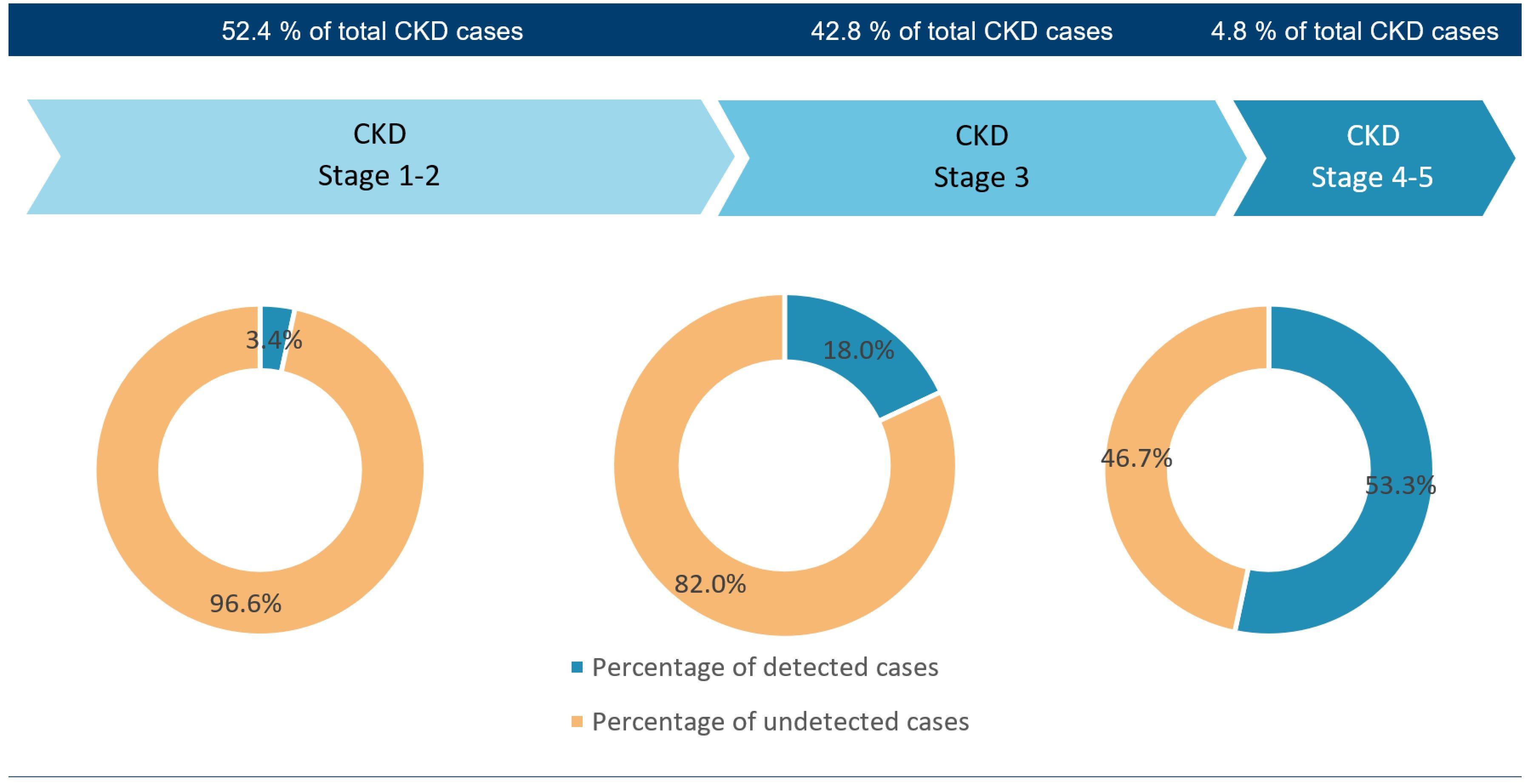
Percentage-wise detection level of CKD with progressing stages
Three-step action plan
Despite the severity of its issues, CKD is not sufficiently prioritized in health policies worldwide. As per Global Kidney Health Atlas, national strategies are required to improve the condition of CKD care and management is still lacking in most countries. To reduce the mortality rate, including the associated risk of cardiovascular deaths, and the financial burden on health systems, effective strategies are required for early detection, prevention, and effective management to slow the progression of the disease in high-risk patients. The following three-step action can help with this:
- Empowerment of medical practitioners: There is a notable shortage of physicians with CKD care specialization across the world. Hence, more healthcare professionals should be empowered with resources to step up and for effective management of CKD. At the same time, multidisciplinary groups should be developed by encouraging and empowering primary care physicians with the necessary resources to alleviate the burden on hospitals and the health system.
- Early detection and prevention of CKD: With simple and inexpensive tests of blood (serum/ plasma) and urine, CKD can be easily detected. The tests calculate the estimated glomerular filtration rate and albumin to creatinine ratio for the early detection and staging of CKD. Current inventions have made the tests easily accessible to people at home or in clinics through point-of-care devices. Based on geography and considering the genetic risk factors and exposures, people with diabetes, hypertension, and heart disease are always at higher risk of developing CKD. As the chart above depicts, most of the CKD cases are diagnosed in the final stages even today. Hence, more focus should be given to early detection of the health status and prevention of the disease in early stages.
- Utilization of digital solutions for care management and delaying progression: For remote and specific rural areas, technological advancements and digital health solutions ease the strain of CKD by improving patient care accessibility while indirectly reducing the overload on healthcare infrastructure. Digital health inventions and continuous collaboration would form the backbone of the system, in which patients would take more control and play an active role in their health. In addition, innovative designs in urban healthcare systems with patient registries and health status indicators are highly essential to identify the accurate stages of CKD. This can be possible only by leveraging digital health solutions so progression can be further delayed with appropriate measures and medications.
Conclusion
CKD can be treated at lower cost and with better outcomes. One of the major drawbacks of the existing healthcare system is lack of early action, as clearly seen in CKD cases. Once CKD progression advances to kidney failure, patients are exposed to many severe health issues that break down the resilience of the system. Nation-wide strategies are needed to tackle CKD by developing early detection programs, enrolling high-risk patients, and monitoring their progress through effective care and management.
